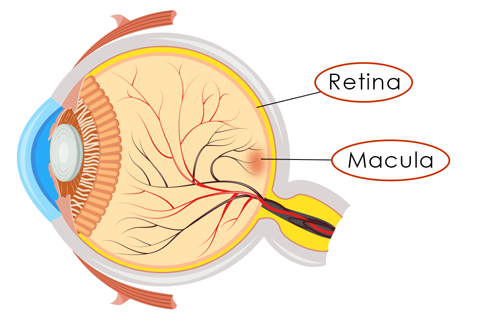
Diabetic Retinopathy
Diabetic Retinopathy encompasses the diabetic eye diseases affecting the retina, the thin lining at the back of the eye which allows images to transmit to the brain. These eye conditions include
nonproliferative retinopathy, macular edema, macular ischemia, and proliferative retinopathy. Diabetic patients are also 60% more likely to develop cataracts, and 40% more prone to glaucoma.5 These conditions affect the front part of the eye.
Diabetic eye diseases occur when the blood vessels in the retina change. They can become damaged and begin to leak fluid and blood into your eye (nonproliferative) or new, abnormal blood vessels develop damaging your retina (proliferative). The leaking and swelling can cause other conditions with the macula such as macular edema. Since the early stages of diabetic eye disease often do not have symptoms, the disease may develop before you realize there has been a change in your eye health. Controlling blood sugar levels with diabetes is extremely important in preserving your vision. Yearly, dilated eye exams are necessary to monitor the affect your diabetes may be having on your vision.

Diabetes and Your Vision
Risk of Diabetic Retinopathy
If you have type 1, type 2, or gestational diabetes, you have issues in how your body either produces or uses insulin. Insulin is a necessary hormone created by the pancreas to deliver glucose (sugar) from the bloodstream to your body to use for energy.
When your body does not use or produce insulin properly, it needs to be provided via injections or an insulin pump. It is necessary to monitor your body’s glucose levels to administer the proper amount of insulin. Without sufficient insulin, your body’s blood sugar levels rise too high causing hyperglycemia. Hyperglycemia causes damage throughout your body, including the small blood vessels of the retina in the eyes.
If you have any type of diabetes, you are at risk of vision loss due to diabetic retinopathy. Factors that can increase this risk include:
- Duration of diabetes
- High blood glucose levels
- High blood pressure
- High cholesterol levels
Prevention of Diabetic Retinopathy
One in two people with diabetes are undiagnosed making them susceptible to health conditions related to diabetes, including diabetic eye disease.^ As with many eye conditions, early detection, timely treatment, and appropriate follow-up care can help save your vision.
Although there is still no cure for diabetes, it is possible to slow its progression and its affect on your vision:
- Control glucose levels, cholesterol, and blood pressure
- Maintain a healthy weight and diet
- Establish an exercise regimen
- Schedule regular health screenings
- Don’t smoke
Studies have shown that diabetics that control blood sugar levels, blood pressure, and cholesterol are four times less likely to experience retinopathy.3 It is possible to have beginning stages of diabetic eye disease and not notice a decrease in vision which is why you should see an optometrist or ophthalmologist at least once a year for a dilated eye exam.
%
of adults with diabetes are undiagnosed!^
diabetic adults have diabetic retinopathy^
%
of type 2 diabetes cases can be prevented^
Two Main Stages of Diabetic Retinopathy
When diabetes is not controlled through medication, diet, and exercise, hyperglycemia occurs allowing glucose to accumulate in the blood vessels. This accumulation damages the small blood vessels that nourish the retina and can cause leakage, swelling, blockage, or development of new abnormal blood vessels in the retina ultimately affecting your vision.
The early or mild stage, NPDR, occurs when the damaged blood vessels within the retina leak blood or fluid causing the retina to swell or form fatty deposits called “exudates”.
When the swelling affects the macula, the area at the center of the retina that provides your pinpoint vision, it is called Diabetic macular edema (DME).
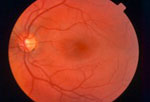
Healthy Retina
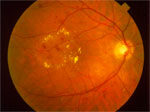
NPDR Retina
Diabetic Macular Edema (DME)
Vision loss is typically not noticed with mild NPDR but when the leaked fluid causes swelling in the retina, the macula can be affected. DME, when the tiny blood vessels within the retina leak blood or fluid, is the most common cause of vision loss with diabetes.4
When the blood vessels of the retina become damaged or blocked in the stages of NPDR, your eye responds with neovascularization. Neovascularization is the growth of new abnormal blood vessels and scar tissue on the surface of the retina prompted by your body’s natural growth hormone and can cause you to see floating spots in your vision. This advanced stage of the disease is proliferative diabetic retinopathy (PDR) and can lead to serious conditions, such as retinal detachment and severe vision loss.

Healthy Retina
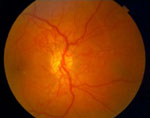
PDR Retina
Effects of PDR
These new abnormal blood vessels are weak and can cause a vitreous hemorrhage, bleeding into the clear, gel-like substance inside the eye. Small amounts of bleeding can cause you to see dark floaters, significant bleeding can block all vision. When bleeding occurs in the center of the eye, scar tissue can form, pull on the retina, and cause a retinal detachment. If the blood vessels grow on the iris they can clog the drainage system of the eye and lead to neovascular glaucoma.6,7
Symptoms
Typically the early stages of NPDR do not have symptoms allowing the disease to become quite advanced before affecting your vision. When the retinal blood vessels leak fluid you may notice blank spots in your vision or blurry central vision. Vision changes may occur in one or both of your eyes. Other symptoms include:
- Blurry vision
- Double vision
- The appearance of spots or “floaters”
- A shadow across the field of vision
- Difficulty reading
- Eye pain or pressure
- Unable to see things in peripheral vision
- Eyes may appear red
- Difficulty identifying colors
Since diabetic retinopathy is not symptomatic until the disease has progressed, if you have diabetes you should have a dilated eye exam annually to detect any changes in the retina before you notice a decline in your vision.
Diagnosis
Regular, dilated eye exams are key in diagnosing any form of diabetic eye disease. During a dilated eye exam, drops are used to widen your pupil. This allows Dr. Westrich and Dr. Krummenacher to use a special lens and look through to the back of the eye at the retina and macula.
They will be looking for signs of:
- Swelling of the macula (macular edema)
- Evidence of poor blood flow to the retina (ischemia)
- Abnormal blood vessels
- Development of new blood vessels (PDR)
Optical coherence tomography (OCT)“] is another way to look at changes to the retina. An OCT uses light waves to take high resolution images of the retina.
A fluorescein angiogram may also be indicated to further examine the retina. Fluorescein is a yellow dye that is injected into a vein in your arm. A special camera takes photos of the retina as the dye travels through the blood vessels and highlights any leakage, blockage, or development of new abnormal blood vessels.
Treating Nonproliferative and Proliferative Diabetic Retinopathy
Intravitreal Injections for Diabetic Eye Disease
Intravitreal injections are an in-office treatment for macular edema. Steroid or “Anti-VEGF” medications are injected into the eye to reduce the swelling of the macula.
Vascular endothelial growth factor (VEGF) is a chemical in the body which stimulates growth of new blood vessels. While VEGF is needed in our bodies, when triggered by the effects of diabetic retinopathy, it can be vision threatening because it creates abnormal blood vessels behind the retina which leak blood and fluid into the retinal layers.
Anti-VEGF drugs are currently the most common and effective treatment for age-related macular degeneration (AMD). Studies have shown these AMD drugs have also proven beneficial in reducing diabetic macular edema. With this treatment, an anti-VEGF drug, such as Lucentis, Eylea, or Avastin, is injected into the eye with a very fine needle. The drug inhibits the development or leaking of the abnormal blood vessels slowing vision loss. These ongoing treatments have proven to reduce DME from diabetic retinopathy and preserve your vision.
Laser Therapy for Diabetic Eye Disease
Laser therapy is an in-office treatment for macular edema. With this procedure, a laser focuses on damaged areas of the retina to reduce fluid leakage and swelling caused by the abnormal blood vessels. The main purpose of this treatment is to prevent further vision loss. It is not possible to gain vision that has already been lost due to diabetic eye disease.
Pan-Retinal Photocoagulation (PRP) for Diabetic Eye Disease
Pan-Retinal Photocoagulation (PR) is an in-office laser treatment for PDR. A laser focuses on all parts of the retina, except the macula, causing abnormal new blood vessels to shrink. This treatment also helps prevent future growth and decreases the chance bleeding and retinal distortion will occur. Multiple treatments are indicated. PRP does not cure PDR but can help prevent further vision loss.
The best treatment for diabetic eye disease is to prevent the development of retinopathy through strict control of your blood sugar.
Diabetes and Your Vision
Diabetic retinopathy is the leading cause of irreversible blindness in working-age Americans.6 Early detection through annual dilated eye exams and timely treatment are the best ways to protect your vision from diabetic eye disease. The National Eye Institute recommends you keep your health on TRACK:
- Take your medications as prescribed by your doctor
- Reach and maintain a healthy weight
- Add physical activity to your day
- Control your ABCs: A1C, Blood Pressure, and Cholesterol
- Kick the smoking habit
Help Spread The Word About Diabetes
Many organizations help educate citizens on the growing health concerns posed by both type 1 and type 2 diabetes. The International Diabetes Federation (IDF) and the World Health Organization created World Diabetes Day on November 14 as an official United Nations Day to help build awareness of this disease. More than 640 million of us may be living with diabetes by 2040.9

D•R•E•A•M of a Cure
- Demonstrate to those around you the benefits of a healthy diet.
- Rejuvinate your body through regular exercise.
- Educate family and friends on the importance of a healthy lifestyle.
- Advocate for diabetes awareness and slow the rise of the disease.
- Motivate those close to you to take charge of their health and A-B-Cs!
“The prevalence of both type 1 and type 2 diabetes is increasing, despite the fact that many cases of type 2 diabetes can be delayed or prevented.”9
-Professor Nam Han Cho
Chair, IDF Diabetes Atlas Committee, 7th Ed.
SOURCES / REFERENCES:
^ “Eyes On Diabetes: Facts & Figures.” International Diabetes Federation, Web. Accessed May 2017.
1 “Eye Complications.” American Diabetes Association, Web.
2 “Facts About Diabetic Eye Disease: Who is at risk for diabetic retinopathy?.” National Eye Institute, Web. Sep 2015.
3 “Eye Care.” American Diabetes Association (ADA), Web. April 2015.
4 “What Is Diabetic Retinopathy.” American Academy of Ophthalmology (AAO), Web. Accessed May 2017.
5 “Glaucoma, Cataracts.” American Diabetes Association (ADA), Web. November 2013.
6 “Diabetic Retinopathy.” American Society of Retina Specialists (ASRS), Web. Accessed May 2017.
7 Diabetic Retinopathy: A Closer Look.. American Academy of Ophthalmology (AAO), Brochure. Copyright 2009.
8 “Healthy ABCs.” American Diabetes Association (ADA), Web. February 2015.
9 “IDF Diabetes Atlas: Seventh Edition.” International Diabetes Federation, Web. 2015.
Other resources include: AAO, National Eye Institute.
![]()


