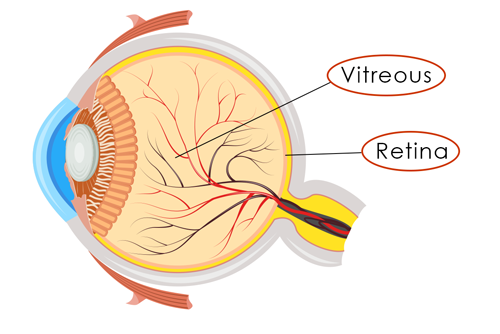
Retinal Tear and Retinal Detachment
Retinal tear and retinal detachment affect the retina, the thin, light-sensitive lining at the back of the eye responsible for transmitting images to the brain. A retinal tear occurs when the retina is pulled away from its normal position. If fluid passes through the tear, it can cause the retina to separate from the back of the eye causing a “detached retina” which can be serious and lead to permanent vision loss.
Our eyes are filled with a gel-like substance called vitreous. The vitreous, which is loosely attached to the retina, thickens, shrinks, and moves away from the retina as we get older. This may cause “floating” specs to appear in our vision. This occurrence is not cause for alarm unless the vitreous pulls on the retina hard enough to cause a retinal tear or retinal detachment. A sudden decrease in vision, increased floaters, sudden flashes of light, and shadows in your peripheral vision can indicate a tear is occurring. During a retinal detachment, it may appear as if a curtain is closing on your vision. These retinal tear and retinal detachment symptoms should be treated immediately to prevent serious vision loss.
Risks of Retinal Tear or Retinal Detachment
A retinal detachment can happen at any age but tend to be more common after age 40. You may be at a higher risk of retinal detachment if you:
- Are extremely nearsighted
- Have already had a previous retinal detachment in your other eye
- Have had previous eye surgery such as cataract
- Have had a serious eye injury
- Are diabetic (new blood vessels may grow under the retina causing a detachment)
- Have or show a family history of lattice degeneration, a thinning the peripheral retina
- Have inflammation or swelling
If you have risk factors or have a family history of retinal issues, regular dilated exams can help monitor the health of your eyes and use preventative treatment to avoid a retinal detachment. Always wear eye protection when playing contact sports and see an eye doctor immediately if an eye injury occurs and affects your vision.
Three Types of Retinal Detachment
- Rhegmatogenous: The most common type of retinal detachment, a rhegmatogenous (reg-ma-TAH-jenous) detachment, occurs when a tear or break in the retina allows fluid to leak under the retina and separates it from the back of your eye. This can happen as a part of aging or occasionally from an eye injury.
- Tractional: Less common, a tractional tear occurs when scar tissue on the surface of the retina causes it to separate from the back of the eye. This type of detachment may result from diabetes or other eye conditions.
- Exudative: Also less common, an exudative retinal detachment forms when fluid leaks of out blood vessels and accumulates under the retina.
Retinal Detachment
Many conditions can lead to a retinal detachment causing the retina to separate from the back of the eye, much like wallpaper peeling off a wall. A retinal detachment requires emergent surgery. When flashes and floaters appear, or a curtain begins to come down over the vision, a retinal surgeon will need to repair the tear or detachment as soon as possible.
Symptoms of a Retinal Detachment
- A sudden increase in the number of “floaters” in your vision which may appear as specks, cobwebs, squiggly lines in your vision
- A sudden appearance of flashes of light
- A shadow or curtain appears in your peripheral vision or moves into the center of vision
- A sudden decrease in vision
Diagnosing a Retinal Detachment
The severity of symptoms is often related to the extent of the tear or detachment. It is possible for a retina to be detaching without changes in your vision which is why regular eye exams are important. The sooner an ophthalmologist diagnoses and treats a retinal detachment, the better the chances of preserving your vision.
In general 9 out of 10 retinal detachment cases are successful but more than one procedure may be indicated.~
Treating a Retinal Detachment
Scleral Buckle
Scleral buckle surgery is an outpatient procedure where the surgeon places a flexible, silicone band around the outside of the eye. This band gently presses the wall of the eye closer to the retinal tear to close the tear. Fluid under the detached retina is drained if necessary to allow the retina to settle back into its normal position against the back wall of the eye. A freezing treatment (cryopexy) or laser treatment (photocoagulation) induces controlled scarring around the tear to seal the damaged area. The buckle will typically remain on the eye permanently.
Pneumatic Retinopexy
Pneumatic retinopexy can sometimes be an in-office procedure. Dr. Westrich or Dr. Metelitsina injects a gas bubble into the inside of the eyeball. The gas bubble pushes the retinal tear back into place against the wall of the eye. Then either a laser treatment (photocoagulation) or freezing treatment (cryotherapy) repairs the tear and prevents further damage to the retina. You will need to maintain a specific head position for several days to keep the gas bubble over the retinal tear as it heals.
Vitrectomy
Vitrectomy surgery is an outpatient procedure. Your surgeon will make an incision in the sclera, the white part of the eye, and remove the vitreous gel, the jelly-like fluid inside the eye. The vitreous is replaced with a gas bubble which will push the retina back in place. A freezing treatment (cryotherapy) or laser treatment, (photocoagulation) is used to repair the damaged area of the retina. You will need to maintain a specific head position as the eye heals and replaces the gas bubble with your body’s natural fluids. A vitrectomy may sometimes be combined with a scleral buckle.
SOURCES / REFERENCES:
^Gretchyn Bailey; reviewed by Vance Thompson, MD. “Detached Retina.” All About Vision, Nov. 2013, www.allaboutvision.com/conditions/retinadetach.htm. Accessed Sep. 2017.
~Retinal Detachment. American Society of Retina Specialists (ASRS), Web.
Facts About Retinal Detachment.” National Eye Institute (NEI), Web. May 2013.
Retinal Detachment: Torn or Detached Retina.” American Academy of Ophthalmology (AAO).
![]()

